- Home
- About Us
- DKPS Dealing
- BLOG
- Delhi NCR
- Delhi
- Physiotherapy at Home Near Me | Physiotherapist in South Delhi
- Best Chiropractor in Delhi
- Physiotherapist in Delhi
- Cupping Therapy in Delhi
- Home Nursing Services in Delhi
- Needle Therapy for Back Pain
- Sports Injury Physiotherapy
- Best Physiotherapist Visit at Home in Rohini Sector 24
- Physiotherapy at Home In Rohini Sector 9 |
- Physiotherapist in Pitampura | Physiotherapy at Home in Pitampura
- Physiotherapy at home in Rohini sector 29
- Physiotherapist in Paschim Vihar
- Physio home visit | Home Visit Physiotherapy |
- Physiotherapist in Saket | Best Physiotherapist in Saket |
- Physiotherapist In Janakpuri | Best Physiotherapist in Janakpuri |
- Best Physiotherapist in Punjabi Bagh | Punjabi Bagh Physiotherapist |
- Best Physiotherapist Service at Home in Dwarka, Delhi
- Best Physiotherapist in Chandigarh at Home Visit
- Faridabad
- Gurugram
- Noida
- Best Physiotherapy Gorakhpur
- Best Physiotherapist in Lucknow | Physiotherapist in Lucknow near me |
- Delhi
- Mumbai
- Delhi NCR
- Department
- Doctors
- Gallery
- Packages
- Contact Us
- Home
- About Us
- DKPS Dealing
- BLOG
- Delhi NCR
- Delhi
- Physiotherapy at Home Near Me | Physiotherapist in South Delhi
- Best Chiropractor in Delhi
- Physiotherapist in Delhi
- Cupping Therapy in Delhi
- Home Nursing Services in Delhi
- Needle Therapy for Back Pain
- Sports Injury Physiotherapy
- Best Physiotherapist Visit at Home in Rohini Sector 24
- Physiotherapy at Home In Rohini Sector 9 |
- Physiotherapist in Pitampura | Physiotherapy at Home in Pitampura
- Physiotherapy at home in Rohini sector 29
- Physiotherapist in Paschim Vihar
- Physio home visit | Home Visit Physiotherapy |
- Physiotherapist in Saket | Best Physiotherapist in Saket |
- Physiotherapist In Janakpuri | Best Physiotherapist in Janakpuri |
- Best Physiotherapist in Punjabi Bagh | Punjabi Bagh Physiotherapist |
- Best Physiotherapist Service at Home in Dwarka, Delhi
- Best Physiotherapist in Chandigarh at Home Visit
- Faridabad
- Gurugram
- Noida
- Best Physiotherapy Gorakhpur
- Best Physiotherapist in Lucknow | Physiotherapist in Lucknow near me |
- Delhi
- Mumbai
- Delhi NCR
- Department
- Doctors
- Gallery
- Packages
- Contact Us
VARICOSE VEINS
- Home
- VARICOSE VEINS
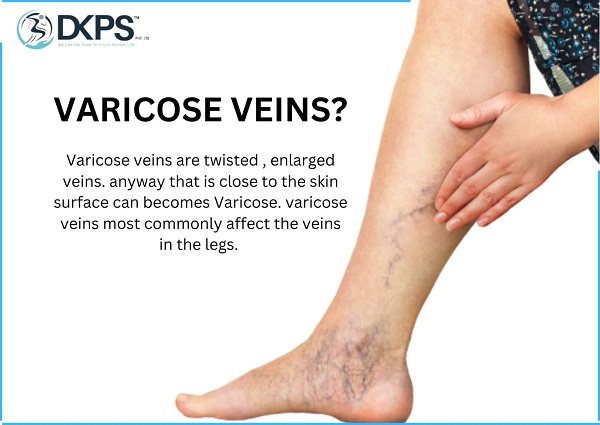
VARICOSE VEINS :
What are the varicose veins?
Varicose veins are enlarged and twisted veins. Varicose veins can occur anywhere on the body but are most common in the legs.
They are not considered serious medical conditions. But, they can be uncomfortable and lead to more serious problems. And because they can be very noticeable, they can make people feel uncomfortable or embarrassed.
Varicose veins, also known as varicose, are a medical condition in which superficial veins become enlarged and twisted. These veins typically develop in the legs, just under the skin. Varicose veins usually cause few symptoms. However, some individuals may experience fatigue or pain in the area, Complications can include bleeding or superficial thrombophlebitis. Varices in the scrotum are known as varicocele, while those around the anus are known as hemorrhoids. The various physical, social, and psychological effects of varicose veins, can negatively affect one’s quality of life. They have no specific cause. Risk factors include obesity, lack of exercise, leg trauma, and family history of the condition. They also develop more commonly in pregnancy Underlying causes include weak or damaged valves in the veins. They are typically diagnosed by examination, including observation by ultrasound. spider veins affect the capillaries. Treatment may involve lifestyle changes or medical procedures with the goal of improving symptoms and appearance. Lifestyle changes may include wearing compression stockings, exercising, elevating the legs, and weight loss. Possible medical procedures include sclerotherapy, laser surgery, and vein stripping. Reoccurrence is common following treatment.
Varicose veins are very common, affecting about 35% of people at some time in their lives. They become more common with age. Women develop varicose veins about twice as often as men. Varicose veins have been described throughout history and have been treated with surgery since at least.
Signs And Symptoms?
*Aching, heavy legs
*The appearance of spider veins telangiectasia in the affected leg Ankle swelling
*A brownish-yellow shiny skin discoloration near the affected veins.
*Muscle cramps when making sudden movements, such as standing.
*Abnormal bleeding or healing time for injuries in the affected area
*Lipodermatosclerosis or shrinking skin near the ankles.
*Atrophied Blanche, or white, scar-like formations.
*Redness, dryness, and itchiness of areas of skin termed stasis dermatitis or venous eczema.
*Burning or throbbing sensation in the legs.
*A positive D-dimer blood test result due to chronic low-level thrombosis within dilated veins varies.
Causes :
Varicose veins are more common in women than in men and are linked with heredity. Other related factors are pregnancy, leg injury, prolonged standing, obesity, and abdominal straining. They are unlikely to be caused by crossing the legs or ankles. Less commonly, but not exceptionally, varicose veins can be due to other causes, such as post-phlebitic obstruction or incontinence, and venous and arteriovenous malformations. Venous reflux is a significant cause. Research has also shown the importance of pelvic vein reflux (PVR) in the development of varicose veins. Varicose veins in the legs could be due to ovarian vein reflux. Both ovarian and internal iliac vein reflux cause leg varicose veins. This condition affects 14% of women with varicose veins or 20% of women who have had a vaginal delivery and have leg varicose veins. In addition, evidence suggests that failing to look for and treat pelvic vein reflux can be a cause of recurrent varicose veins. It could also be caused by hyperhomocysteinemia in the body, which can degrade and inhibit the formation of the three main structural components of the artery: collagen, elastin, and proteoglycans. Homocysteine permanently degrades cysteine disulfide bridges and lysine amino acid residues in proteins, gradually affecting function and structure. Simply put, homocysteine is a ‘corrosive’ of long-living proteins, etc. collagen or elastin, or lifelong proteins. These long-term effects are difficult to establish in clinical trials focusing on groups with existing artery decline. Parkes-Weber syndrome is relevant for differential diagnosis
Arteries carry blood from the heart to other parts of the body, and arteries return blood from the rest of the body to the heart. To return blood to the heart, the veins of the legs must fight against gravity. This blood flow is controlled by valves. These valves in the arteries open as blood flow to the heart and then close to prevent blood from flowing back, this happens when the muscle acts as a pump and the elastic walls of the arteries help blood return to the heart. heart. If the valve becomes weak or damaged, as with varicose veins, blood can back up and pool in the vein, causing it to stretch or twist.
Physiotherapy treatment for varicose veins :
*Compression:
Wearing compression stockings is important to prevent and treat varicose veins. They squeeze your legs regularly to help improve your posture. They can also help reduce pain, discomfort, or swelling in the feet.
walking:
Just take a walk. This is a great way to stimulate blood circulation in your feet.
*Legs Lift:
To perform a leg lift, the patient sits or lies on their back with their legs extended. Then the patient lifts one leg at a time, holding it in the air. Lower it slowly and repeat the same exercise with the other leg.
*knee bends:
Lie on your back again on the floor. Slowly draw one knee into your chest, holding your leg behind your knee (holding above the knee puts undue pressure on this delicate joint). Now, point and flex your foot several times. Do this slowly and forcefully – don’t let your leg flop loose, but tighten the calf muscles and the tendons around your ankle. repeat with the opposite leg
*Swimming:
Swimming pushes blocked blood in the legs and helps with varicose veins. The posture of a person while swimming is horizontal, which increases blood flow in the legs. It is a simple form of physiotherapy that can be done sitting or standing.
Find more related articles :
DKPS Physiotherapy Services at home in city :
DELHI | NOIDA | GREATER NOIDA | GHAZIABAD | FARIDABAD | GURGAON | MUMBAI | PUNE | NASIK | NAVI MUMBAI | GUWAHATI | LUCKNOW | HYDERABAD | KANPUR | GORAKHPUR | HARIDWAR | VRINDAVAN | MATHURA | MANY MORE |
Other Places where we provide Physiotherapy Services at Home
- Physiotherapy at home in Rohini sector 24
- Physiotherapy at home in Rohini
- Physiotherapy at home in Budh vihar
- Physiotherapy at home in pitampura
- Physiotherapy at home in Panjabi bagh
- Physiotherapy at home in Rani bagh
- Physiotherapy at home in Ashok vihar
- Physiotherapy at home in shastri nagar Delhi
- Physiotherapy at home in inderlok Delhi
- Physiotherapy at home in kanhaiya Nagar Delhi
- Physiotherapy at home in paschim vihar
- Physiotherapy at home in Vikas Puri
- Physiotherapy at home in Karol bagh
- Physiotherapy at home in Rajendra place delhi
- Physiotherapy at home in Patel Nagar Delhi
- Physiotherapy at home in Shadipur delhi
- Physiotherapy at home in Kirti Nagar Delhi
- Physiotherapy at home in moti nagar Delhi
- Physiotherapy at home in Noida
- Physiotherapy at home in Gaziyabad
- Physiotherapy at home in Gurgaon
- Physiotherapy at home in Faridabad
- Physiotherapy at home in burari
- Physiotherapy at home in sangam vihar
- Physiotherapy at home in Gandhi vihar
- Physiotherapy at home in mukherjee nagar
- Physiotherapy at home in jagatpur village
- Physiotherapy at home in gopalpur
- Physiotherapy at home in civil line
- Physiotherapy at home in delhi university
- Physiotherapy at home in Mumbai
- Physiotherapy at home in GTB nagar
- Physiotherapy at home in model town
- Physiotherapy at home in kamla nagar
- Physiotherapy at home in nirankari colony
- Physiotherapy at home in Chauhanpatti
- Physiotherapy at home at khjuri khas
- Physiotherapy at home in Bhajanpura
- Physiotherapy at home in Ankur vihar
- Physiotherapy at home in tronica city
- Physiotherapy at home in Jhaghirpuri
- Physiotherapy at home in Okhla delhi
- Physiotherapy at home in shaeen bagh delhi
- Physiotherapy at home in houz khash Delhi
- Physiotherapy at home in Narela delhi
